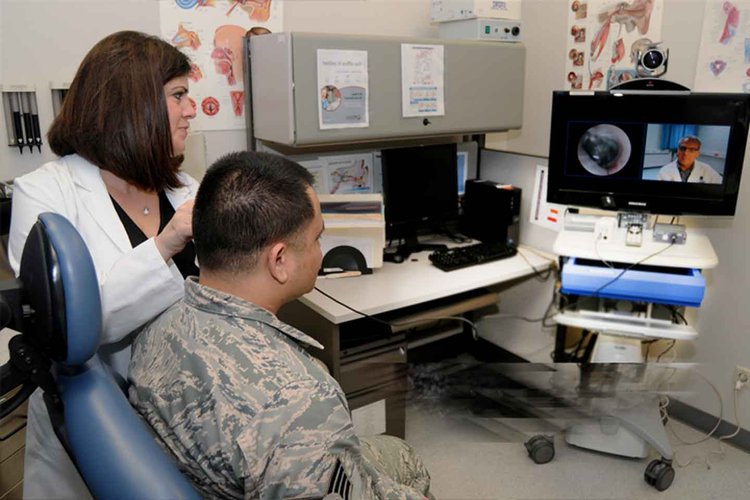
Many American military veterans are seeing medical specialists today without leaving their primary care doctors’ offices—or even their own homes. In 2015, in fact, 677,000 veterans received some of their care remotely through telehealth. That comes to 12% of the 5.6 million people the U.S. Department of Veterans Affairs (VA) provides care for each year.
“The VA is recognized as a leader in the development and use of telehealth technology,” Kevin Galpin, MD, executive director of telehealth services for the Veterans Health Administration, told a Senate Appropriations subcommittee in May, while asking Congress to increase the investment in telehealth in 2018.
A major advantage of telehealth is that it offers access and convenience. Telehealth can connect providers with patients who live in rural or remote areas, where there may not be many specialists, for instance. About 45% of VA telehealth patients live in rural areas, according to Galpin.
“Making a vet travel three hours on a recurring basis for care is impractical,” said Scott Shipman, MD, MPH, the AAMC’s director of primary care initiatives and workforce analysis. A study at the VA medical center in White River Junction, Vt., concluded that telehealth can save 142 minutes of driving per visit.
“Mental health care often carries a stigma, which can lead to missed appointments and lower-quality care.... If you can conduct [a mental health visit] with a provider via video in the comfort of your own home, it can reduce that stigma and improve care.”
Scott Shipman, MD, MPH
AAMC
Telehealth can also ease travel for patients with mobility issues no matter where they live, Galpin added. Then add the cost savings benefit. The estimated annual savings for each patient enrolled in the Veterans Health Administration’s telehealth program averaged $6,500 in 2012, or a total of $1 billion, according to a 2014 case study.
In addition to remote clinical services, telehealth technology is used to provide remote training and continuing medical education for staff and students. Medical trainees now get telemedicine experience at the Denver Department of Veterans Affairs Medical Center and other institutions. Some of the VA’s experience in telehealth is being adapted by the Indiana University School of Medicine and the University of North Dakota School of Medicine and Health Science.
When hands-on treatment is not essential
Academic medical centers have another important role in telehealth: Assessing its quality and teaching students how to use it.
Telehealth can be particularly advantageous in treating certain conditions. Between 2003 and 2016, the VA reported 1.8 million telehealth visits for mental health care. And one study of 100,000 veterans from 2006 through 2010 showed a 24.2% drop in psychiatric hospitalizations among those who enrolled in a VA telehealth program.
“Mental health patient evaluation and cognitive behavioral therapy can be done very well via high-quality audio and video,” noted Thomas Nesbitt, MD, MPH, interim vice chancellor for human health sciences at the University of California, Davis, and associate vice chancellor for strategic technologies and alliances for the UC Davis School of Medicine.
“Mental health care often carries a stigma, which can lead to missed appointments and lower-quality care, Shipman said. “Telehealth enables this care to be provided in a more discreet manner. If you can conduct [a mental health visit] with a provider via video in the comfort of your own home, it can reduce that stigma and improve care.” A recent randomized study of vets treated for posttraumatic stress disorder (PTSD) over six months showed no arguable difference in outcomes between those treated in person versus those treated via telehealth.
Another area lending itself to telehealth is HIV care, said Michael Ohl, MD, MSPH, of the Iowa City VA Health Care System and lead investigator on a study to improve rural veterans’ access to HIV care through telehealth. The 800 Texas and Georgia veterans enrolled in the study live near primary care clinics but face a 90-minute drive to the nearest specialty clinic for HIV. The study is finding that most HIV-affected rural vets will take the telehealth option.
Telehealth works well for patients whose HIV is well controlled, said Ohl. “If someone is acutely ill, or has very advanced HIV infection with AIDS, we generally try to see them in person if we can.
[But] there are cases where people live a long way away, don’t have transportation, and they just can’t get to us. We prefer active face-to-face if they have issues going on, but telehealth is better than no care.”
Nesbitt stressed that the value of telehealth is as an additional tool in health care delivery. “I prefer to use telehealth as a supplement rather than as a substitute. People should have a coordinated [in-person] relationship with their care team.”