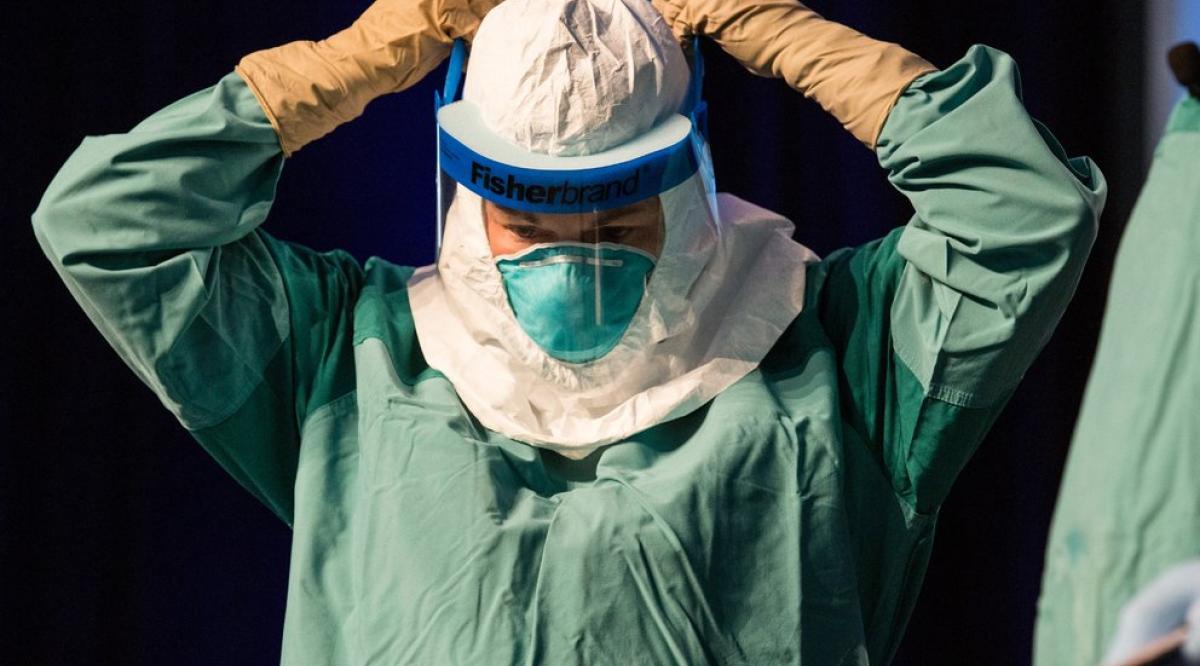
This week, the Democratic Republic of the Congo announced that 33 people had died in recent days of Ebola, just weeks after declaring an earlier outbreak contained. In 2014, when the virus infected several U.S. citizens, we were woefully unprepared. Here is what has happened since.
Imagine a doctor in a U.S. hospital treating an Ebola patient. The clinic is chaotic and loud, and the patient is vomiting, covered in bloody emesis. The doctor studies the scene. She needs to make life-or-death decisions. How should she respond?
This is one of multiple likely scenarios in the University of Nebraska Medical Center’s (UNMC) upcoming virtual reality room — part of a new $118.9 million, 190,000-square-foot training facility opening in May 2019. The VR room will simulate almost any environment, from a smoke-filled terrorist attack to a hurricane-ravaged town, allowing healthcare professionals to perform triage, provide emergency care, or make decisions about transporting patients. How realistic is it? For the Ebola scenario, an odor simulator will allow doctors and nurses to, yes, smell the vomit.
The staff at UNMC understand the need for Ebola training. During the outbreak in West Africa in 2014, only three U.S. facilities had operational biocontainment units (BCUs): UNMC, Emory University Hospital in Atlanta, and the National Institutes of Health in Bethesda, Maryland. (An additional 60 hospitals eventually received CDC clearance to treat Ebola patients.) UNMC received three patients. Two survived, but a third, Martin Salia, MD, arrived with advanced symptoms and died two days later. For both hospitals and the government, the experience was a wake-up call.
“I think everyone knew that we needed to get serious,” says James LeDuc, PhD, director of the Galveston National Laboratory, part of the University of Texas Medical Branch and one of 12 biosafety level 4 labs in the United States. “The government realized we weren’t prepared.”
Today, there are 10 academic medical centers with federally funded BCUs located around the country. And the National Ebola Training and Education Center (NETEC), established in 2015, has provided online and on-site training to hundreds of other hospitals and medical centers in the United States.
“I think the biggest benefit, hands-down, is that any person in this country that becomes ill with Ebola, or any highly infectious disease, has access to a well-prepared treatment center,” says Melissa Harvey, RN, MSPH, director of National Healthcare Preparedness Programs and the Hospital Preparedness Program in the U.S. Department of Health and Human Services’ (HHS) Office of the Assistant Secretary for Preparedness and Response. “And that certainly was not the case prior to 2014.”
Those actions were critical, because the threats have not diminished.
“We have megacities around the world with terrible hygiene and poverty,” says LeDuc, who also serves on the World Health Organization’s (WHO) Global Outbreak Alert and Response Network. “The idea of an infectious disease like Ebola getting started, and repeating what we saw in West Africa, is a worrisome scenario. I think we’re going to continue to see outbreaks and controlling them is going to be exceptionally difficult.”
Last week, the Democratic Republic of the Congo announced that four people had tested positive for Ebola, just days after declaring an earlier outbreak “largely contained.” Should the virus spread globally, it’s fair to ask: Is the United States really better prepared for an Ebola outbreak? The answer is yes, but many Ebola experts worry about a loss of funding that could eliminate much of the progress made over the last four years.
More treatment centers, better collaboration
When Kent Brantly, MD, a U.S. missionary working in Liberia, was admitted to Emory in 2014, he became the United States’ first-ever Ebola patient. Emory had built its BCU in 2002 — it’s the only U.S. hospital certified by WHO to handle smallpox cases — and the staff successfully treated Brantly, fellow missionary Nancy Writebol, and WHO physician Ian Crozier, MD. But while Emory and UNMC could handle a few Ebola patients at a time, most hospitals couldn’t. And when two Dallas nurses became the first U.S.-transmitted cases after treating a man who’d recently traveled to West Africa, government officials began to worry.
In 2015, even before the outbreak had officially been declared contained, HHS allocated $20 million to nine academic medical centers (a tenth was added in 2016), creating a network of regional centers that could provide care for patients with extremely infectious diseases.
That same year, HHS also allocated $12 million to establish the NETEC, a collaboration between three institutions that received Ebola patients in 2014: Emory, UNMC, and Bellevue Hospital Center in New York City. Over its first three years, the NETEC has provided training, hosted education sessions, created a national clinical research network, and developed a massive online resource repository with everything from symptom information to a hospital preparedness checklist. By mid-2018 alone, NETEC representatives had conducted 33 technical assistance visits at hospitals and medical centers around the country (you can request a NETEC readiness consultation online).
In April 2018, the NETEC led the largest patient-movement exercise in HHS’s history — a nationwide effort that involved over 50 organizations, including the U.S. State Department, airport authorities, and emergency management agencies.
The exercise simulated an outbreak in seven remote areas of the country. Patients arrived at a hospital, where they were tested, isolated, then moved to an airport and flown to their respective regional centers (Oklahoma, for example, is in region six; the regional treatment center is the University of Texas Medical Branch).
“These are complex events where you’re coordinating all the transport logistics, with tons of different agency collaboration,” says Shelly Schwedhelm, MSN, RN, NEA-BC, executive director of Emergency Management and Biopreparedness at UNMC.
The participating BCUs and hospitals are preparing their reports on the April exercise, but “the training went great,” says Harvey. Many hospitals found that they needed to clarify their procedures. Would a pediatric patient’s family, for example, be allowed in a BCU? Federal officials learned that even though they want to standardize the government’s coordination role, each region operates differently. “Some regions have the regional treatment center as the lead — they’re coordinating everything from the ground transport to receiving the patient,” says Harvey. “In other regions, that role is played by the state public health department. We learned a lot of lessons.”
The funding conundrum
As effective as these training exercises have been, the concern now is as much about funding as fevers. The five-year funding for the NETEC and the regional treatment centers expires in 2020, and many veterans of 2014 worry that the network will disappear without federal support.
“We were scrambling in 2014 to find facilities beyond Emory and Nebraska,” says Harvey, who notes that federal funding to increase Ebola preparedness will reach $56 million by July 2019 -- $32 million for the regional treatment centers and $24 million for NETEC.
“Now we finally have sufficient capability throughout the country — but that capability isn't going to stay unless we nurture it. I could envision a scenario where there’s an Ebola or Lassa fever outbreak in 2023 and we’re right back where we started.”