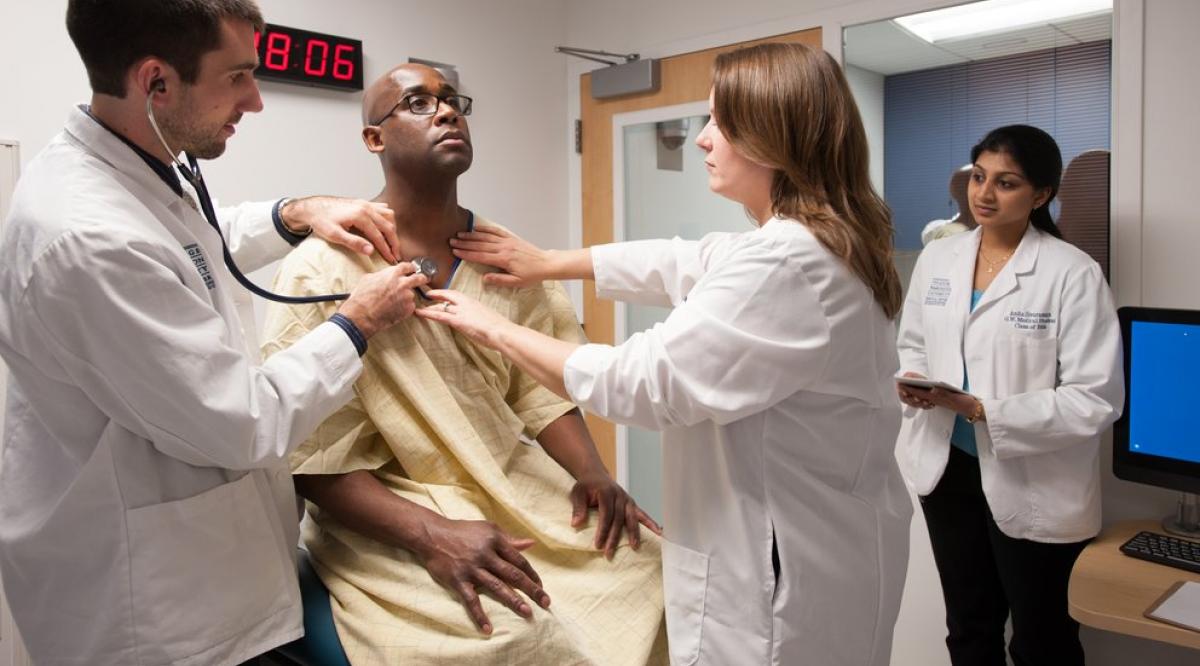
At Columbia University College of Physicians and Surgeons, Jonathan Amiel, MD, and colleagues are revamping how students learn to take a patient history, conduct a physical, make presentations, and document findings.
Amiel, associate dean for curricular affairs at Columbia, is integrating the AAMC’s Core Entrustable Professional Activities for Entering Residency (Core EPAs) into Columbia’s curriculum with the goal of improving a medical graduate’s readiness for residency. Working with program directors others, the AAMC developed the Core EPAs to identify the skills and tasks that new residents should be able to perform on their first day with minimal supervision.
In May 2014, the AAMC published Core Entrustable Professional Activities for Entering Residency, which serves as a guide for curriculum developers, faculty, and learners to better prepare medical students for residency and their future roles as clinicians. The 13 EPAs, which range from taking a patient history to interpreting diagnostic tests to collaborating as part of an interprofessional team, are being piloted at 10 medical schools nationwide.
“I think this is the largest transformation [in medical education] in recent history and one that is poised to make a tremendous impact on the transition from school to residency.”
Jonathan Amiel, MD
Compared with more traditional competencies, which describe the various abilities a physician needs, the Core EPAs represent a group of tasks that all graduates should be ready to do regardless of their specialty, explained Kimberly Lomis, MD, associate dean for undergraduate medical education at Vanderbilt University School of Medicine. She noted that the EPAs are so innovative, in part, because they take traditional competencies and group them in the context of distinct workplace expectations that include trustworthiness.
“We want to help students understand how to shift from trying to get a high grade to explicitly working toward earning our trust,” Lomis said. “The EPA guide makes it very transparent to the learner what we’d like them to attain.”
Next steps
At Columbia, one of the pilot schools, the project has provided an opportunity to reexamine how the school teaches clinical skills longitudinally and how faculty assess students, Amiel said. Ultimately, Amiel wants to build a four-year arc of EPA-based learning that both builds student confidence and provides extra training when necessary.
“EPAs let students know what they’re working toward and how any piece of education is contributing toward their ability to act,” said Amiel, also the principal investigator for the Columbia EPA team. “I think this is the largest transformation [in medical education] in recent history and one that is poised to make a tremendous impact on the transition from school to residency.”
A major goal of the pilot project is to find effective ways to integrate the Core EPAs into curricula and assess whether students may ultimately be entrusted to work without supervision. However, an even bigger and more challenging goal is coming to a shared agreement on standards. “If each school sets different standards for entrustment, residency program directors will not be able to rely upon our assessments,” Lomis said.
If all goes as planned, a portion of the 2019 class at each pilot school will be the first to receive formal assessments in some of the EPAs. In addition, the pilot group has issued a set of Core EPAs Guiding Principles for institutions that intend to use the new framework.
Interest and excitement about the EPAs is growing far beyond the 10 pilot schools. “Those of us lucky to be involved are really excited,” said Eva Aagaard, MD, associate dean for educational strategy and director of the Center for Advancing Professional Excellence and the Academy of Medical Educators at the University of Colorado School of Medicine. “We’re excited about the possibilities the EPAs create, and we see it as a way to solve some big problems around curriculum and assessment.”
Aagaard chairs the Entrustment Learning Community, one of four AAMC learning communities designed to share knowledge and disseminate best practices about the EPAs beyond the initial pilot sites. She described the EPAs as an innovative framework to teach students how individual competencies come together in health care delivery. At the same time, the competencies allow educators to “unpack” a particular EPA to more precisely pinpoint where a student is having trouble, she said.
Currently, the AAMC learning communities are still figuring out how to best engage with the pilot schools and begin distributing lessons learned. “The combination of EPAs and competencies is very helpful in moving us forward in the competency-based education movement,” Aagaard said.
Student feedback
Nathan Friedman, a rising fourth-year student at Vanderbilt, became familiar with the EPAs while working on a research project on informed consent.
During his project, Friedman asked fourth-year medical students to assess their own informed consent skills. Then he compared those answers to assessments from their faculty supervisors. Using the AAMC guidelines on EPAs to analyze the results, Friedman found that underperformers tended to overrate their abilities, while overachievers underrated their abilities.
The results were not surprising, Friedman said, noting that much of the scientific literature on assessment has come to similar conclusions. As a medical student, he said the EPAs offer greater clarity on what will be expected of him as a resident.
“The EPAs give us a way to think about what specific tasks we’re good at and where we need improvement,” Friedman said. “It gives us a target.”
But Friedman did find that using the task-based EPA framework seemed like a more “natural and translatable” way to assess a student’s abilities rather than relying only on graduation competencies, which he said can seem “nebulous and abstract.” He added that knowledge of the EPAs will make him “more appropriately nervous, but more confident about where I need to improve” as he moves toward residency.
“I think coming out of my clinical [clerkship] year, I felt pretty good, but as I’m gaining more exposure to EPAs and learning about the expectations of being an intern, it’s taking my confidence level down a bit,” he said. “But I think that’s a good thing. The EPAs help you keep that learner’s hat on and continue to grow in the fourth year.”