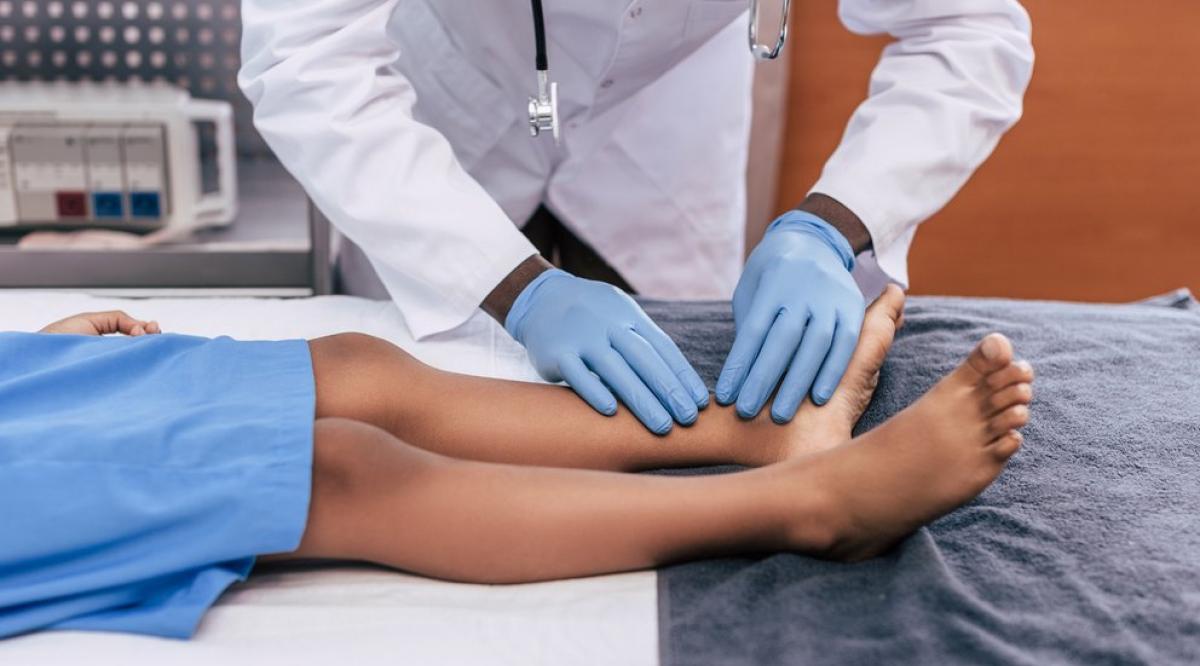
From his first month as a student at the University of Arkansas for Medical Sciences (UAMS) in Little Rock, Ark., Grant Cagle learned how to drape a patient, take a medical history, perform physical exams, deliver bad news, and more. And he was able to learn and practice these clinical skills—and make mistakes—without affecting actual patients.
Nearly all U.S. medical schools now employ standardized patients (SPs), also known as simulated patients or simulated participants. Educators coach these lay people to portray patients in realistic situations as a means to help medical students learn how to grapple with sensitive issues.
In one case, Cagle worked with a woman portraying a Muslim patient trying to control her hypoglycemia as she fasted for Ramadan. “I thought that was really cool,” says Cagle, who grew up in a small Missouri town and had never heard of the holy month.
These “patients” have provided him with helpful feedback, letting him know if he clicked his pen during an office visit, for example. One SP told him, “Grant, you may have been a little short with me when you were counseling me on quitting smoking.” Cagle, now in his fourth year, says, “I couldn’t tell you how amazing this was … it helped calm my fears, it helped me learn how to say things [and avoid hurting patients’ feelings].”
This medical training technique has four key purposes— education, assessment, research, and health system integration— according to the Society for Simulation in Healthcare. This method of learning gives students a safe, controlled setting in which to experience the initial stress, awkwardness, and confusion of office visits; practice ultrasounds; gain exposure to rare events; and build self-confidence. Institutions also use SPs to assess medical students’ clinical competence and interpersonal skills and provide ongoing training to licensed health professionals.
Carefully recruited and trained SPs also participate in one step of the United States Medical Licensing Examination. The simulation program at UAMS uses the same setup that students encounter during the clinical skills component of their medical boards, seeing 12 SPs over nine hours.
Mock exam and operating rooms
The late neurologist and educator Howard Barrows, MD, is credited with originating the SP concept in the 1960s while at the University of Southern California. “It’s extremely effective,” says Lisa Howley, AAMC senior director of strategic initiatives and partnerships and a founding member of the 16-year-old Association of Standardized Patient Educators (ASPE). “Today, SPs are an integral component of our medical education system.”
Many schools connect students with SPs in sophisticated simulation centers set up to replicate operating and exams rooms. Students also carry out complex training scenarios on-site at hospitals, where students can experience a mock code blue—sometimes using realistic, high-fidelity patient mannequins and engaging with SPs who play grieving loved ones. In addition, SPs are frequently used in concert with technical simulators to enhance the learner experience and facilitate patient safety.
“I think the thing I’ve been most grateful for is the sense of confidence that [SPs] gave me as a provider.”
Dorothy “Jet” Patterson
University of Arkansas for Medical Sciences
“If students see a patient in a clinic on this campus, they see us first,” says Mary Cantrell, executive director of the UAMS Centers for Simulation Education. The university’s simulation program, which started in Cantrell’s living room in 1992, now includes a core of 200 SPs, 14 staff members, and the Center for Clinical Skills Education, a 4,000-square-foot facility with 14 exam rooms.
“I think the thing I’ve been most grateful for is the sense of confidence that [SPs] gave me as a provider,” says third-year UAMS student Dorothy “Jet” Patterson. “Sometimes I’ll walk into a room and completely forget that it’s a standardized patient.” One SP, for instance, portrayed someone with gallbladder pain. “I was really concerned for her and completely forgot [she was an SP],” she recalls.
Second-year UAMS students encounter the complicated patient, such as a woman who is crying because she just received a breast cancer diagnosis or a patient who dislikes the doctor. “Students tend to always remember the angry man,” says Cantrell. Working with SPs also helps students practice navigating an exam room: raising examining tables, moving stools, finding things.

Carolinas HealthCare System’s simulation center in Charlotte has 19 full-time staff members and works with nearly 100 SPs to provide scenarios for University of North Carolina medical students and for the system’s residents and health care professionals.
“We’re a system resource, like a library,” says Carolinas Simulation Center Director Dawn Swiderski. In addition to introducing medical students to physical exams, SPs at the center help skilled nursing staff practice interpersonal skills and early sepsis identification. For disaster preparedness and mass-casualty influx training, they play hurricane or mass-shooting victims. The center also uses SPs in research, including a new safety skills study focused on residents handing off patient information.
According to Swiderski, students learn how to talk and make eye contact with patients and become aware of their own idiosyncrasies. “When you’re nervous, do you talk with your hands, do you say ‘um’ a lot?” she says. Working with SPs, as well as the system’s nursing, ethics, and pastoral care staff, also teaches students how to handle code scenarios, the aftermath of a significant medical error and the very important task of how to convey bad news.
The simulation center’s mock operating, exam, and labor and delivery rooms are fitted with one-way mirrors and a control room, which can’t be seen. Classmates watch a live stream as students or residents work with SPs, then the class comes together for a debriefing. “That peer-to-peer input actually does wonders to solidify learning,” notes Swiderski.
Being an SP is tough work
UAMS has trained 45 lay people to teach medical students how to perform various exams on their bodies, including gynecological and male genitourinary checks. These teaching associates undergo six months of training and earn more than the standard SP. UAMS pays standardized patients about $16 an hour, but those participating in rigorous cases—cases requiring them “to cry a lot and act like their husbands have died”—get paid time and a half, says Cantrell.

Scott Wilson, who heads the Carolinas SP program, explains that Carolinas’ SPs range in age from 18 to 80. “They come in all shapes and sizes,” he says, and include off-duty EMTs, nurses, actors between plays, and other professionals.
“Sometimes the nonverbal behaviors of the health care team that they are the least aware of will have the most effect on the patient,” says Mary Donovan, administrative director of Georgetown University School of Medicine’s SP program and a former SP herself.
Roughly 20 years ago at Johns Hopkins University School of Medicine, Donovan portrayed the sister of a dying accident victim. She and her “brother-in-law” had to decide whether to consent to donating the patient’s organs.
“That was tough work ... [and] a very emotional experience,” Donovan remembers. The players were offered psychological counseling.
“Sometimes the nonverbal behaviors of the health care team that they are the least aware of will have the most effect on the patient.”
Mary Donovan
Georgetown University School of Medicine
Georgetown employs more than 100 of the roughly 300 SPs who work among seven medical schools in the Baltimore–Washington, D.C., area, using 40 or 50 of them fairly regularly, says Donovan. In addition to other exercises, Georgetown medical students encounter four SPs portraying angry, crying, terse, and overly chatty patients—all within two hours.
Depending on case needs, SPs can put in anywhere from eight to hundreds of hours a year, according to Donovan. They must play a “specific and repeatable patient,” accurately recall the encounter, score clinical and communication skills on checklists for most events, and learn how to provide constructive interpersonal feedback, she explains. “If you haven’t done this work, it’s hard to appreciate what [SPs] are expected to do, reliably and consistently.”
ASPE recently published standards of best practice for those working with these human role players. Research has shown that SP training produces positive results for health professionals and patients. The Carolinas Simulation Center, for example, participated in a training initiative using SPs that aimed to reduce hospital readmissions for skilled nursing facility patients. EMS systems data showed that the facilities saw up to a 35% reduction in EMS transports after the training, notes Wilson.
“We’re protecting real patients, in a way, through the use of simulated patients,” says Howley. “We’re protecting our learners and better preparing our learners for their work.”