When health care disparities are highlighted, insurance access and inability to pay often take the spotlight. But health coverage can be just one obstacle in a series of health care barriers. An insurance card in your wallet does not automatically alleviate the many hurdles to receiving care, said Philip Alberti, PhD, AAMC senior director for health equity research and policy.
"Insurance does not equal access. Access does not equal utilization. Utilization does not equal quality, and quality does not equal equity," said Alberti. For example, even before the Affordable Care Act’s insurance expansions took effect, insured Hispanic adults were more likely to lack a usual provider of care than insured white and black adults, according to a 2015 study by the Commonwealth Fund.
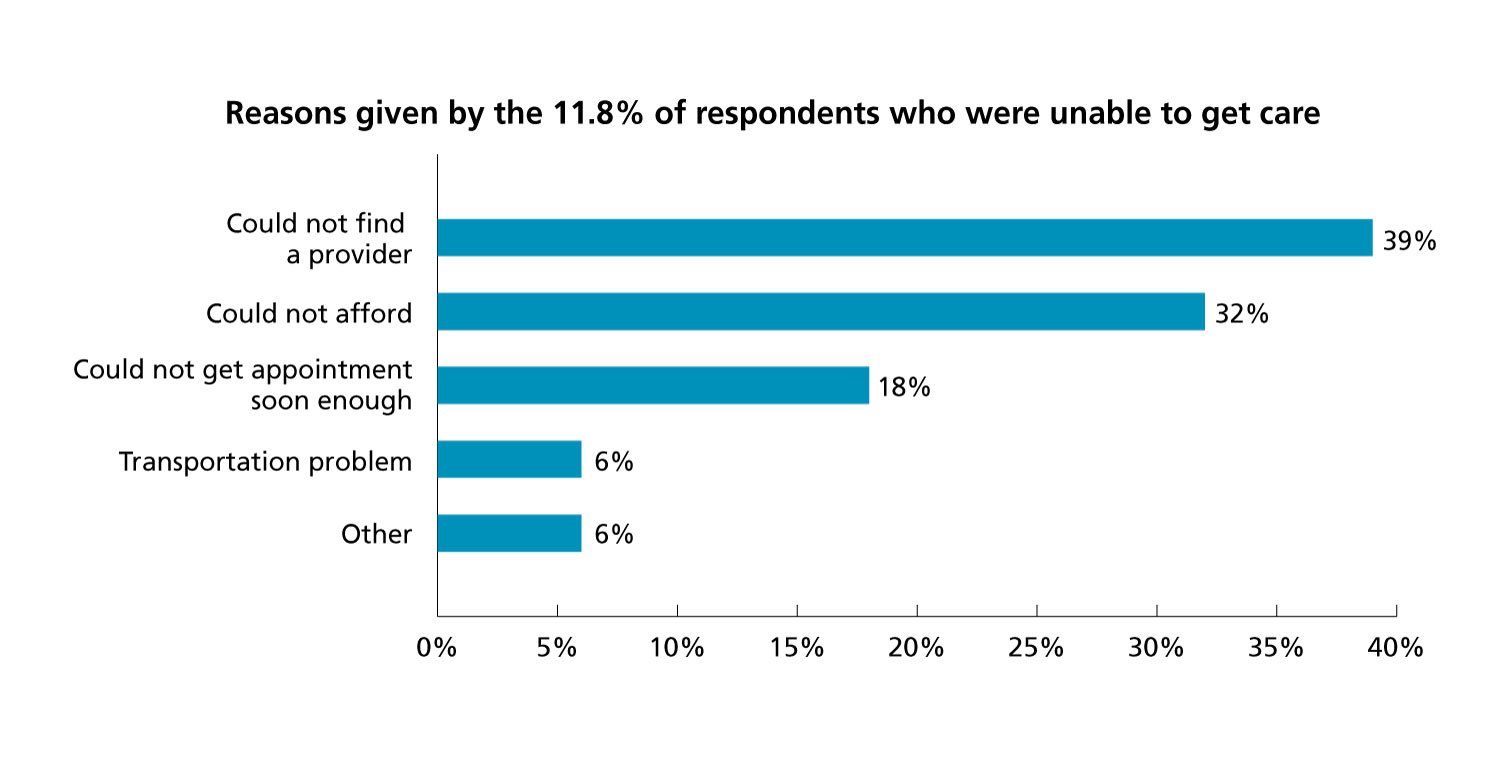
Among the less visible factors affecting health care access are those referred to as the social determinants of health. These determinants include socioeconomic status, education, physical environment, employment, and social support networks. While cost is a significant factor in people’s inability to access health care, a survey by AAMC Workforce Studies (below) showed it wasn’t the most frequently reported reason.
Addressing these influences by gathering more data, learning how to increase the reach of interventions, and moving beyond disease-focused approaches is part of the next wave of health equity research, said Lisa A. Cooper, MD, MPH, vice president for health care equity for Johns Hopkins Medicine and professor of medicine at Johns Hopkins University School of Medicine. For tomorrow’s doctors, she added, it’s important to teach them how to reduce health disparities—not just that they exist.
Deciphering data behind disparities
At the Johns Hopkins Center to Eliminate Cardiovascular Health Disparities, multidisciplinary teams use implementation science and community-based participatory research to target health disparities and build ties among researchers, providers, community members, and policymakers. “By engaging with the community, we are able to see firsthand the kinds of problems that affect our most vulnerable populations and then hear possible solutions from those same people,” said Cooper, who is director of the center.
Investigators at the center recently completed a clinical trial exploring racial disparities in blood pressure control, long known to be an issue in the black community. The trial, called Project ReDCHiP (Reducing Disparities and Controlling Hypertension in Primary Care), analyzed health-system and clinic-level factors affecting implementation, quality improvement, and disparity reduction across six practices in Baltimore that serve racially diverse patients.
Interventions identified from the trial to improve outcomes for these patients included blood pressure measurement training for staff, patient care management that targets dietary strategies and medication adherence, and teaching clinicians to use health information technology to enhance communication with patients.
After employing the interventions, researchers saw a dramatic reduction in the proportion of recorded blood pressures with a terminal zero, suggesting high use of automated devices. In addition, blood pressure control improved for black and white patients who participated in a few sessions of care management, and patients rated their experiences with the program as very positive, according to Cooper. Upcoming studies will build on the analysis, she added.
Boots on the ground boost community care
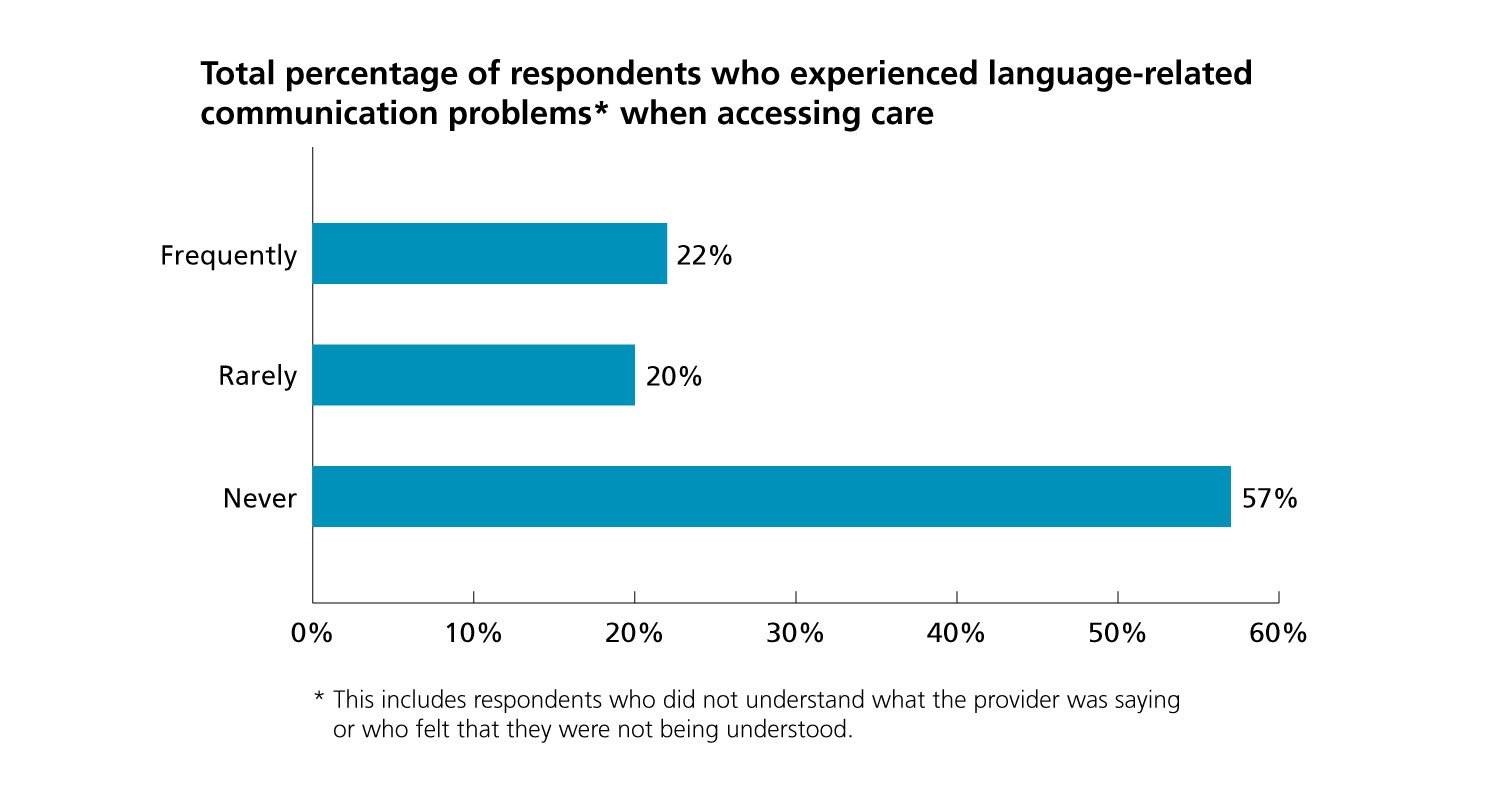
Medical students at the Chicago Medical School at Rosalind Franklin University of Medicine and Science are helping to address health disparities in a predominately Spanish-speaking community near Chicago. Students launched a community clinic about four years ago to serve this population, said Jeanette Morrison, MD, Chicago Medical School senior associate dean for student affairs and education. Competent use of language and effective communication are at the center of strong physician-patient relationships, research has shown, and barriers in language can keep some patients from seeking care.
“Academic medical centers need to continue thinking about how they can move their efforts upstream in partnership with communities, public health agencies, departments of education, transportation, and urban planning.”
Philip Alberti, PhD
Association of American Medical Colleges
The university's Interprofessional Community Clinic is a joint collaboration between medical students and students from other disciplines, such as podiatry, physical therapy, pharmacology, and nursing. The partnership enables patients to access multiple health services in one place and receive referrals for ongoing care. “The patient benefit is tremendous,” said Morrison.
For some patients, transportation is as much a barrier as language differences or finances. So, the community clinic took to the road, said Gordon Pullen, PhD, assistant dean for basic science education at Chicago Medical School. Students and clinicians staff a mobile clinic, which travels to places in North Chicago and Waukegan to provide health care.
“Students get to care for patients they might not ever know are out there in the community,” said Morrison. “They get the opportunity to work with an interpreter. They get to learn some medical Spanish. It’s a real eye-opener for them.”
MedStar Health and Hackensack University Health Network have taken another innovative approach to helping people without private transportation. Both institutions have partnered with Uber to help patients get to their medical appointments.
Partnerships build bridges, fill gaps
Similar efforts to combat health disparities have led the University of Colorado School of Medicine at the Anschutz Medical Campus (CU School of Medicine) to establish a free clinic for indigent Aurora residents. The Dedicated to Aurora’s Wellness and Needs (DAWN) clinic provides integrated primary care and serves as a patient-centered medical home for uninsured patients, said Lynn M. VanderWielen, PhD, MPH, an assistant professor in the Department of Family Medicine at the CU School of Medicine. Partnerships of health profession schools and free clinics remain underused, she wrote in a 2015 article in Medical Education Online.
The DAWN clinic started in 2014 as a collaboration with the Colorado chapter of Primary Care Progress, a national group dedicated to accelerating advancements in primary care. The clinic staff includes licensed and credentialed volunteer providers, as well as precept student volunteers from various CU health profession schools. “Research in this area suggests that these opportunities challenge students to critically examine the interplay of social conditions and health and often result in the pursuit of careers in primary care and/or underserved communities,” VanderWielen said.
Beyond the clinic, the CU School of Medicine is working in partnership with the Mental Health Center of Denver toward the creation of a community panel that will target health disparities. The panel will include members from communities with unequal social and economic conditions, said VanderWielen, who is leading the effort in collaboration with the Center for African American Health and the Colorado Department of Public Health and Environment.
“Academic medical centers need to continue thinking about how they can move their efforts upstream in partnership with communities, public health agencies, departments of education, transportation, and urban planning,” Alberti summed up. “Now more than ever, when there is so much uncertainty about the future of the 20-plus million newly insured Americans, [it’s a good time for] academic medical centers to examine the many health barriers beyond insurance coverage and start working to eliminate such obstacles.”
The AAMC Consumer Survey of Health Care Access, 2016
This data, prepared by AAMC Workforce Studies, includes responses from 5,932 U.S. adults who needed or received medical care in 2016.